Nutrition and Sickle Cell Disease: Foods that Help and Foods to Avoid
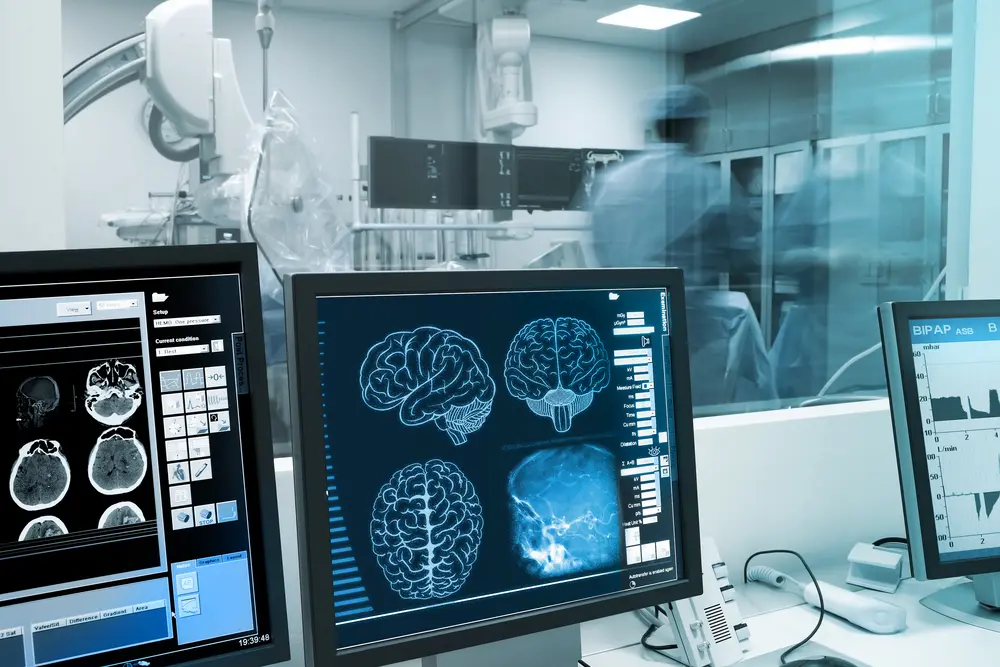
Sickle Cell Disease (SCD) is a genetic blood disorder that affects the shape and function of red blood cells. Instead of being round and flexible, like healthy red blood cells, the cells in someone with SCD are crescent or "sickle" shaped. The change in shape causes these cells to get stuck in blood vessels, leading to painful episodes known as crises and other serious health issues like stroke, eye problems, infections, chronic pain, chest pain, and shortness of breath.
Living with SCD is tough, but the proper nutrition can help. The right foods can help your body produce healthier red blood cells, reduce pain and inflammation, and give you the energy you need to feel your best.
Understanding Sickle Cell Disease
SCD is a genetic blood disorder that’s marked by flawed hemoglobin (hb). Hb is the protein in the red blood cells that transports oxygen to the body tissues. SCD interferes with the delivery of oxygen to the tissues.
What Causes Sickle Cell Disease?
SCD is inherited in an autosomal recessive pattern, meaning a person must inherit two abnormal hemoglobin genes (one from each parent) to develop the disease. If someone inherits one abnormal gene and one normal gene, they will have sickle cell trait, which typically doesn't cause symptoms of SCD but can be passed on to offspring. Risk factors include:
- Family history of sickle cell disease
- People who are African Americans or from Middle Eastern, Mediterranean, and Indian ancestry
- Genetic inheritance
Signs and Symptoms of Sickle Cell Disease
Signs and symptoms of SCD can include:
- Anemia
- Acute chest syndrome
- Pain crisis (sickle crisis)
- Splenic sequestration (pooling)
- Jaundice
- Priapism
Please note that these symptoms vary in intensity and require prompt medical attention when severe. Symptoms like acute chest syndrome, where sickle cells block vessels in the lungs and cause chest pain, fever, and breathing difficulty, can be life-threatening. So, it’s critical to work closely with your healthcare provider to monitor and address these symptoms as they arise.
SCD Diagnosis
Diagnosis is done early in life with a newborn screening. This test checks for the presence of sickle hemoglobin shortly after birth. Early diagnosis is super important because it lets doctors start treatment right away to prevent complications. If you are pregnant and suspect that you, your partner, or both of you have the sickle cell trait, genetic counseling can help clarify the situation and provide guidance on the potential risks for your child.
Sickle Cell Disease Treatment
SCD is a lifelong disease. Most treatments are designed to help improve quality of life, though options like bone marrow transfer have been shown to potentially cure SCD:
- Pain management, which involves the use of medications to relieve pain during sickle cell crises.
- Hydroxyurea, a medication that helps reduce the frequency of pain episodes and other complications.
- Blood transfusions, to help increase healthy red blood cells and prevent complications like stroke.
- Bone marrow transplant, which involves replacing diseased bone marrow with healthy marrow from a donor.
Foods that Help Improve Health in Sickle Cell Diseas

A healthy diet supplies the body with the nutrients it needs to fight infections and promote health. Here are some great goods to integrate as part of your diet when you have sickle cell disease:
Fluids
Hydration is good for the body, even under normal circumstances. But it’s critical when you have sickle cell. Your body needs fluids to keep the blood flowing smoothly and prevent sickle cells from clumping together. Go for at least eight glasses of water a day. Herbal teas and natural fruit juices without added sugars are also great choices.
Iron-Rich Foods
Iron is super important because it helps your body make healthy red blood cells, which helps fight anemia – a common issue with SCD. Try to include the following foods and pair them with foods rich in Vitamin C (bell peppers or oranges) for better absorption.
- Fish: Especially sardines and salmon
- Leafy greens: Like spinach, kale, and Swiss chard
- Lean meats: Like beef, chicken, and turkey
- Legumes: Including lentils, beans, and chickpeas
Folate-Rich Foods
Folate also does a great job helping the body produce red blood cells. Great examples of folate-rich foods are:
- Leafy greens: Spinach, collard greens, broccoli, and romaine lettuce
- Citrus fruits: Oranges, lemons, and grapefruits
- Beans and peas: Black-eyed peas and kidney beans
- Fortified cereals and breads
Antioxidant-Rich Foods
Such foods help reduce oxidative stress and inflammation, which is beneficial for SCD. These foods, rich antioxidants, can help protect your cells and support your immune system:
- Berries: Blueberries, strawberries, and raspberries
- Seeds and nuts: Almonds, walnuts, and sunflower seeds
- Colorful vegetables: Including carrots, bell peppers, and broccoli
- Green tea
Omega-3 Fatty Acids
These foods have anti-inflammatory properties that can help reduce pain and improve your overall health. They also are good for your heart health. Foods rich in omega-3s include:
- Fatty fish: Like salmon, mackerel, and sardines
- Flaxseeds and chia seeds
- Walnuts
- Soybeans
Protein-Rich Foods
Proteins help your body repair and grow, which is great for SCD. Make sure to get a variety of protein sources:
- Lean meats and poultry: Chicken and turkey are good options.
- Fish and seafood: Rich in protein and often in omega-3s.
- Eggs: A versatile and complete protein source.
- Dairy products: Milk, cheese, and yogurt provide both protein and calcium.
- Plant-based proteins: Tofu, tempeh, and edamame are excellent for variety. Plant-based proteins: Including tofu, tempeh, and edamame
Foods to Avoid if You Have Sickle Cell Disease

Just as there are foods that can help you feel better with sickle cell disease, there are also foods that might make your symptoms worse. Here are some types of foods you should try to avoid:
High-Sodium Foods
Foods high in sodium can increase your blood pressure and cause your body to hold onto extra fluids. This puts more strain on your heart and blood vessels. Lower your sodium intake to help keep your heart and blood vessels healthy.
Gluten
Foods rich in gluten tend to worsen anemia. Gluten may damage the intestinal wall and limit folic and iron absorption, which are essential in the production of red blood cells.
High-Fat Foods
Unhealthy fats, especially saturated and trans fats, cause inflammation and increase the risk of heart disease. It's important to maintain a healthy weight and manage your cholesterol levels to keep your heart in good shape.
Caffeine and Alcohol
Limit or avoid caffeine and alcohol intake. Caffeine contains tannins which bind to iron molecules and interfere with iron absorption in the body. Alcohol affects the production and maturation of red blood cells, causing abnormality or dysfunction of cells. It also affects how nutrients are absorbed from food and may lead to folic and iron deficiencies. Until recently, a bone marrow transplant was the only cure. But in December 2023, two new therapies got FDA approval to treat sickle cell disease. One approach involves adding a gene to the body, while the other modifies an existing gene. Clinical trials are also exploring gene-based treatments alongside other therapies to help reduce symptoms and extend lifespan.